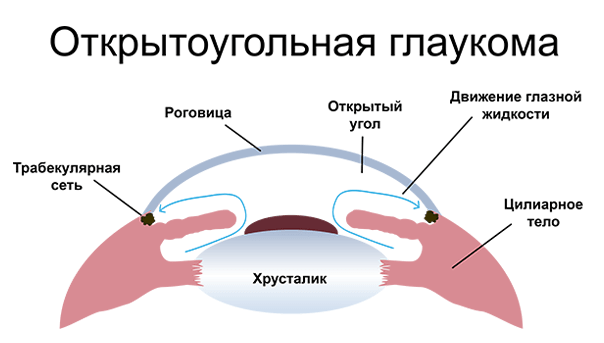
Open-angle glaucoma refers to damage to the optic nerve and loss of visual function where the angle of the anterior eye chamber remains open.
World statistics show that glaucoma is the second cause of irreversible blindness after cataracts. Among the two types of this condition, open-angle glaucoma is more frequent than closed-angle glaucoma.
This pathology significantly reduces the quality of life, worsens the psycho-emotional and physical condition.
Open-angle glaucoma in both eyes is particularly dangerous because it leads to total irreversible vision loss. Early diagnosis and timely treatment are the key to a favorable outcome for the patient.
Eximer Ophthalmology Clinic specializes in treating various degrees of open-angle glaucoma. We offer modern diagnostic methods, individual treatment plans, and operations with state-of-the-art medical equipment.
The main risk factor for glaucoma is high intraocular pressure, which can be corrected.
Causes of occurrence
As we live, there is a constant fluid inflow and outflow in the eye. It is expelled through the drainage system by an open angle between the iris and the cornea, and the pressure inside the eye is maintained at 18-22 mm Hg.
If the circulation is disturbed, the fluid accumulates in the eye and begins to press on its internal structures. In particular, high pressure affects the optic nerve, which slowly dies out, the brain does not receive signals from it, and vision loss occurs as a result.
High intraocular pressure (IOP) in glaucoma results from abnormalities in the drainage system of the eye. These disorders may be very different. Therefore, when open-angle glaucoma develops, its causes fall into two large groups:
Primary open-angle glaucoma
It occurs as an independent pathology and mostly develops with age. The key patient group is aged over 50. The angle of the eye chamber gradually occludes, the first unpleasant symptoms appear, and IOP gradually increases. There are risk factors in which primary open-angle glaucoma develops more frequently:
- Age over 50 years old, and patients over 60 have the disease 6 times more often than in other age categories;
- Family history. The risk of occurrence increases fivefold if family members have had the pathology;
- High blood pressure.
Secondary open-angle glaucoma
Secondary open-angle glaucoma is caused by occlusion of the anterior chamber angle due to external and internal factors:
- Treatment with steroids and certain hormones increases the risk by up to 40%;
- Trauma, burns;
- Concomitant pathologies such as diabetes mellitus, cataracts, other endocrine disorders.
In rare cases, congenital open-angle glaucoma occurs in infants due to peculiarities of intrauterine development. For example, underdevelopment of the angle of the ocular chamber, vorticose veins, closure of the angle by mesodermal tissue, and others.
Symptoms of open-angle glaucoma
Glaucoma symptoms largely depend on the degree of damage to the optic nerve and may not appear at early stages. In most cases, a person notices disturbances in the visual fields when the optic nerve is severely damaged. Asymmetric impairment further aggravates the situation. If one eye is healthy, the other is not able to see clearly.
Initially, this condition starts with the loss of the visual field from the nose, gradually extending to the paracentral parts below and above.
When open-angle glaucoma actively develops, the symptoms do not last long:
- Feeling of grittiness, pain, and heaviness in the affected eye;
- Reduced visual fields. The person sees as if “through binoculars” (lateral external vision persists for a long time until the terminal stage);
- Blurred vision;
- Decrease in twilight vision;
- Watery eyes;
- Colored halos around the light source.
If the intraocular pressure increases significantly with glaucoma, additional symptoms may arise:
- Pain in the temples, eyebrow area, and the eyes themselves, especially in the evening;
- Migraines extending into the eye area;
- Red eyes with dilated congestive vessels, but no burst vessels;
- After moving into darkness, such as a dark room, visibility is dramatically impaired, vision takes a long time to adapt and normalizes only after a few minutes.
Stages of open-angle glaucoma
The International Classification of Diseases defines 4 degrees (stages) of glaucoma according to the signs of optic atrophy:
- Stage 1 glaucoma, or initial glaucoma;
- Stage 2 glaucoma — developing process;
- Stage 3 glaucoma — advanced process;
- Stage 4 glaucoma — terminal or blindness.
Another classification splits the condition into groups based on IOP (intraocular pressure):
- Normal IOP, below 21 mm Hg;
- Moderately elevated IOP (22-28 mm Hg);
- High IOP, over 29 mm Hg.
Accordingly, several types of the condition may be defined, which characterize its progress and risk:
| First degree | Second degree | Third degree | Fourth degree | |
| А | 1A – initial process with minimal changes, usually without subjective symptoms | 2A – the process is developing, but IOP is within the normal range | 3A – there is atrophy of the optic nerve with normal IOP | 4A – blindness |
| В | 1B – initial process without significant changes in the optic nerve, but with (with initial changes in the central visual field and optic nerve head), increased IOP | Open-angle glaucoma 2B. The process is developing dynamically, increased IOP, there are changes in the optic nerve and visual fields | 3B, 3C – changes in the optic nerve are clearly expressed, visual fields are disturbed, pain and discomfort are felt in the eyes due to high IOP | 4B, 4C – blindness with increased or high IOP |
| C | 1C – no serious changes in the optic nerve and visual fields, while very high IOP, which is manifested by unpleasant symptoms | 2C – there are visible changes in the optic nerve, IOP is high. Impaired visual function, there is soreness and other symptoms of glaucoma |
Diagnosis
Early diagnosis of glaucoma is extremely important. The earlier the pathology is detected, the easier it is to control it. This is why it is imperative to visit an ophthalmologist once a year even if there are no expressed symptoms. If glaucoma has been observed in the family history, it is worth seeing an ophthalmologist every six months. It is urgent to visit the doctor if there is a pain in the eyes and narrowing of the visual fields.
An eye exam allows determining the disease at once. If open-angle glaucoma is suspected, diagnosis may consist of several methods:
- IOP determination (tonometry);
- Tonography to study intraocular fluid outflow;
- Determination of the visual fields;
- Examination of the eye ground;
- Determination of the degree of excavation and thickness of nerve fibers with optical coherence tomography.
Medications for open-angle glaucoma
With open-angle glaucoma, medications are limited to eye drops of two types:
- Drugs to reduce intraocular fluid secretion;
- Drugs to increase the drainage function.
Such treatment is effective in the early stages, but it presents several issues:
- The drops cause significant side effects such as nausea, fatigue, itchy eyes, blurred vision, tachycardia, and others.
- The drops need to be put in every day and at the same time! You should not skip doses!
- High-cost therapy. Drugs are not cheap, and they are needed regularly.
- Regular check-ups with an ophthalmologist are required.
Medications may control the glaucoma progression and relieve symptoms, but they do not eliminate the cause of glaucoma. Surgery is required to restore normal drainage and fluid circulation.
Glaucoma treatment at Eximer Ophthalmology Clinic
Open-angle glaucoma is treated at Eximer Ophthalmology Clinic using state-of-the-art technologies such as lasers, valve systems, fluid filtration devices.
The following surgeries are performed for open-angle glaucoma:
Laser trabeculoplasty or selective trabeculoplasty
The main objective is to lower the IOP by eliminating the fluid outflow blockage. The thinnest laser beam affects the trabecular diaphragm (part of the eye drainage system).
Benefits:
- Fast and effective. It takes several minutes, and the effect lasts for months.
- Repeated interventions are possible. The procedure is safe, does not cause significant changes in the eye structures, and can be repeated several times if necessary.
- Painless and bloodless. The recovery period lasts for several days, and there is no open surgery or blood loss during the operation.
Non-penetrating deep sclerectomy
Это хирургическое вмешательство, при котором мембрану роговицы делают тоньше.
This is a surgical procedure to make the corneal membrane thinner.
Benefits:
- Fluid balance is restored naturally by changing the internal eye structures;
- It allows getting rid of glaucoma in its earliest stages when there is no pronounced nerve atrophy yet.
Ex-press fluid filtration device implantation
This method has been used in ophthalmosurgery for over 10 years. The Ex-press device is made of a medical alloy, it is inserted under the scleral flap, and acts as a drain.
Benefits:
- Persistent hypotensive effect;
- Minimal traumatic effect during surgery;
- Fewer check-ups in the postoperative period.
Ahmed Valve implantation
This device is likewise implanted in the eye to control the intraocular pressure by regulating fluid drainage.
Benefits:
- Controlling IOP as the main cause of glaucoma;
- Controlling the number of drops in glaucoma and avoiding too low pressure;
- Effective for all types of glaucoma.
All surgeries at Eximer Ophthalmology Clinic are performed within one day. The patient does not require hospitalization, and the recovery period lasts just several days. Eximer is a leader in ophthalmic surgeries across Ukraine.
Contraindications to surgery and possible complications
A common contraindication to glaucoma surgery is the presence of concomitant eye diseases, as well as a high risk of vision loss that exceeds positive predictions.
Complications after surgery are extremely rare, mostly related to the recovery period and the individual characteristics of the body. In some cases, the drainage holes made to drain the fluid are quickly sutured by new tissue, and repeat surgery is needed.
Ways to live with open-angle glaucoma
If you have been diagnosed with open-angle glaucoma, are being medicated, or are preparing for surgery, you need to adjust some habits.
When living with open-angle glaucoma, contraindications may include:
- Watching TV, gadgets, and reading books in the dark or with a desk lamp; glasses without the necessary correction. The room should be well and evenly lit.
- Sunglasses with dark lenses. If you wear any, give your eyes a break from unnecessary darkness. An alternative is sunglasses with green lenses.
- Frequent prolonged bending and heavy exercises in the gym, which cause a significantly prolonged blood flow to the head. Cycling and tennis are good choices for sports.
- Sudden temperature changes. It is undesirable to stay in a bathhouse, sauna, in the scorching sun.
- Certain medicines. If you are treating other diseases, be sure to tell your doctor about glaucoma.
- Drinking heavily, more than one glass at a time.
- Tight collars and ties worsen blood circulation in the head and neck area and can cause increased intraocular pressure.
The remaining activities fit easily into everyday life with glaucoma: drawing, embroidery, reading, but such work should be done in an even light. Don’t forget to visit your ophthalmologist and follow all the instructions!