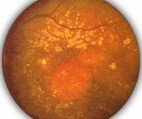
What is the retina?
The retina is the thinnest inner membrane of the eye, which adjoins the vitreous body on the inside and the vascular membrane on the outside of the eyeball.
Its intricate structure allows the retina to perceive light, process and transform light energy into a nerve impulse. This is a signal that encodes all information about what the eye sees and transmits it through the optic nerve to the brain.
The retina consists of receptor cells called rods and cones. Rods are highly sensitive to light and allow you to see in the dark. They are also responsible for peripheral vision. Cones require more light to work, but they are responsible for central vision and allow you to see small details and distinguish colors.
The major part of the retina is the central one called the macula. The macula is opposite the pupil, just above where the eye meets the optic nerve. It gets its other name (yellow spot) because of the yellow pigment in its cells. In the central area, the retina is very thin and contains a large number of cones. It is the macula that is responsible for central vision, so disorders in this area of the retina can lead to significant visual impairment up to blindness.
Risks of retinal diseases
Retinal diseases are considered among the deadliest of all visual impairments because they can lead to complete and irreversible vision loss.
Retinal abnormalities are gradually becoming the leading cause of incurable blindness in middle- and high-income countries. The consequences of retinal diseases are of great concern to ophthalmologists around the world. While medicine has successfully addressed such eye diseases as cataracts, the treatment of disorders associated with the transmission of nerve impulses to the brain causes serious difficulties. Scientists all over the world are now actively working on the development of an artificial retina, which will be a real breakthrough in ophthalmology. In the meantime, timely diagnosis and monitoring is the only way to successfully cope with retinal diseases and to prevent vision loss.
Retinal diseases may not reveal themselves for some time, but visual impairment and even blindness can come suddenly. Any degenerative process on the retina means that sooner or later you may lose your vision. Therefore, people in the risk group should always undergo regular full diagnostics of the visual system with a thorough examination of the eye ground structures. If the therapy is delayed, surgical intervention is necessary. In this case, it is not about improving vision, but about preserving and stabilizing it at the current level.
When do retinal diseases occur?
Retinal abnormalities can arise in some eye diseases, various general and systemic diseases of the body such as hypertension, diabetes mellitus, kidney and adrenal gland diseases, as well as eye injuries, craniocerebral trauma, age-related and hormonal changes in the body.
The main risk groups include:
- People with moderate to high myopia;
- Pregnant women;
- Elderly people;
- People with diabetes mellitus and hypertension.
Symptoms of retinal diseases:
- Decreased vision for no apparent reason;
- Flashes in the form of sparks, lightning;
- Floating spots in the form of soot flakes;
- Shadows in front of the eyes;
- Some visual fields narrowing and dropping out (usually on the side);
- Migraine, dizziness.
The initial stages of the retinal disease may not be accompanied by any symptoms.
Main types of retinal diseases
Peripheral retinal degenerations
One of the most common retinal disorders is peripheral retinal degeneration. One often does not even suspect that he or she is suffering from the disease. Peripheral degenerations may occur at any age and with any visual acuity, but most often in people with medium to high myopia. With myopia, as a rule, the eyeball is enlarged and the retina is stretched and thinned. Blood flow slows down in the more stretched areas, the retina does not receive nutrients, and degenerative changes occur in this state. Retinal tears and thinning are not uncommon and, if not treated in time, could lead to serious consequences such as retinal detachment.
Statistically, peripheral retinal degenerations develop in myopic people in 30-40% of cases, in farsighted people in 6-8%, and in people with normal vision in 2-5%.
Retinal detachment
Retinal detachment refers to the splitting of the inner membrane of the eye from the vascular one. This disturbs the nutrition of its outer layers and causes rapid death of the photoreceptors. The symptoms include decreased visual acuity, narrowing of the visual field, the appearance of floating spots, flickers, and shadows before the eyes, sudden loss of lateral vision, deformation, and fluctuation of the visible objects under examination. Retinal detachment is an extremely serious disease that almost always leads to irreversible vision loss if treatment is not provided in time. It occurs most often in myopic people, but can also result from trauma or a hypertensive crisis.
Statistically, 72% of all cases of irreversible blindness are caused by retinal detachment.
Age-related macular degeneration (macular dystrophy)
Age-related macular degeneration affects the central part of the retina known as the macula. In most cases (the so-called dry form), the changes are caused by thinning of the macular tissue due to age-related alterations and/or pigment deposition therein, resulting in detachment foci. This impairs the photoreceptor function and vision. The other form of age-related macular degeneration, wet macular degeneration, is associated with abnormal overgrowth of blood vessels below the retina in the macula. They are fragile and often leak blood and fluid that lift the macula from its normal place at the back of the eye. This condition soon leads to pathological changes in this area of the retina. Wet macular dystrophy progresses much faster than its dry form, leading to a dramatic deterioration in vision.
The main risk factors for age-related macular degeneration are age over 50, cardiovascular diseases, and genetic predisposition. In its initial stages, this condition is invisible to the patient and can only be detected at an ophthalmologist’s appointment.
Age-related macular degeneration is the most common cause of vision loss in people over 50.
Diabetic retinopathy
Diabetic retinopathy is a frequent complication of diabetes mellitus. When you have diabetes, there are metabolic disorders due to a lack of insulin, leading to the loss of cells that maintain the tonicity of the walls of small vessels. The weakening of the vascular walls leads to pathological changes, resulting in retinal hemorrhages and abnormal newly formed vessels, which may cause retinal detachment and irreversible vision loss.
Diabetic retinopathy evolves gradually, and even its marked stages can be imperceptible. Diabetic retinopathy usually develops 5 to 10 years after the diabetes onset and leads to blindness if left untreated.
Diabetic retinopathy is found in 40% of diabetic patients.
Macular edema
Macular edema refers to swelling of the central area of the retina, the macula, which is responsible for central vision. Macular edema results from fluid accumulation in the central area of the retina, which significantly reduces visual acuity. Macular edema is not an independent disorder but a symptom of certain eye diseases or conditions such as diabetic retinopathy (retinal vascular lesions caused by diabetes mellitus), eye trauma or postoperative complications, uveitis (inflammation of the choroid), and retinal vein occlusion. Retinal vein occlusion is one of the most dangerous eye pathologies, which can lead to irreversible vision loss.
Retinal disease diagnosis
A simple eye exam is not enough to diagnose the retina. If retinal abnormalities are suspected, the following examinations are mandatory:
- Visual field (perimetry) exams to assess the retina in its periphery;
- Ultrasound examination of the internal structures of the eye;
- Eye ground examination (ophthalmoscopy) to assess the retina, optic disc, and eye ground vessels;
- Optical coherence tomography (OCT) of the retina, enabling us to assess the macular (central) zone.
Ways to react to retinal diseases
The key point in retinal diseases is the timely diagnosis. If retinal pathologies are revealed, it is advisable to undergo regular diagnostic examinations, preferably at the same medical center, and use the same equipment to monitor the retina in dynamics. It is vital to follow all the doctor’s recommendations, including those related to lifestyle, exercise regimen, diet, and so on. Timely treatment can preserve your vision and prevent it from deteriorating.
Retinal disease treatment
There is no all-purpose method of treating retinal diseases. Each case requires an individual approach. When choosing the best method, many factors are taken into account such as the type of disease, its causes, stage, age of the patient, concomitant conditions, and so on. The treatment process remains under the doctor’s control and he or she can make adjustments depending on the results.
Modern ophthalmology benefits from the following methods of treating retinal diseases:
- Laser treatment: laser photocoagulation, PPLC;
- Surgical treatment (vitreoretinal interventions);
- Medications;
- Intraocular injections with Lucentis, Eylea, Ozurdex.
Retina of pregnant women
Hormonal imbalance is typical during pregnancy, which might severely affect eyesight. The main threat to the visual system is the retina. Retinal impairment is one of the most frequent reasons when a natural delivery is miscarried and a cesarean section is recommended. The risk of retinal detachment increases with natural delivery because of the pressure fluctuations of the woman in labor. This risk is particularly high in myopic patients and those prone to retinal abnormalities. Ophthalmologists strongly recommend that all women, regardless of visual acuity, should have an eye exam with eye ground study at weeks 6, 10-14, and 32-36 of pregnancy.
Prophylactic peripheral laser coagulation is used to treat dystrophic changes in the retina and prevent the risk of retinal detachment. This simple procedure is completely safe for both the expectant mother and the baby and is performed until the 36th week of pregnancy.
Retina and myopia
Myopic people should undergo regular eye exams and monitor their retina. However, it is not always related to your myopia degree. Often, with high myopia, the retina is stable and satisfactory, with no tears or progressive dystrophic changes. On the contrary, with low myopia of fewer than 3 diopters, dystrophic foci can be seen on the eye ground.